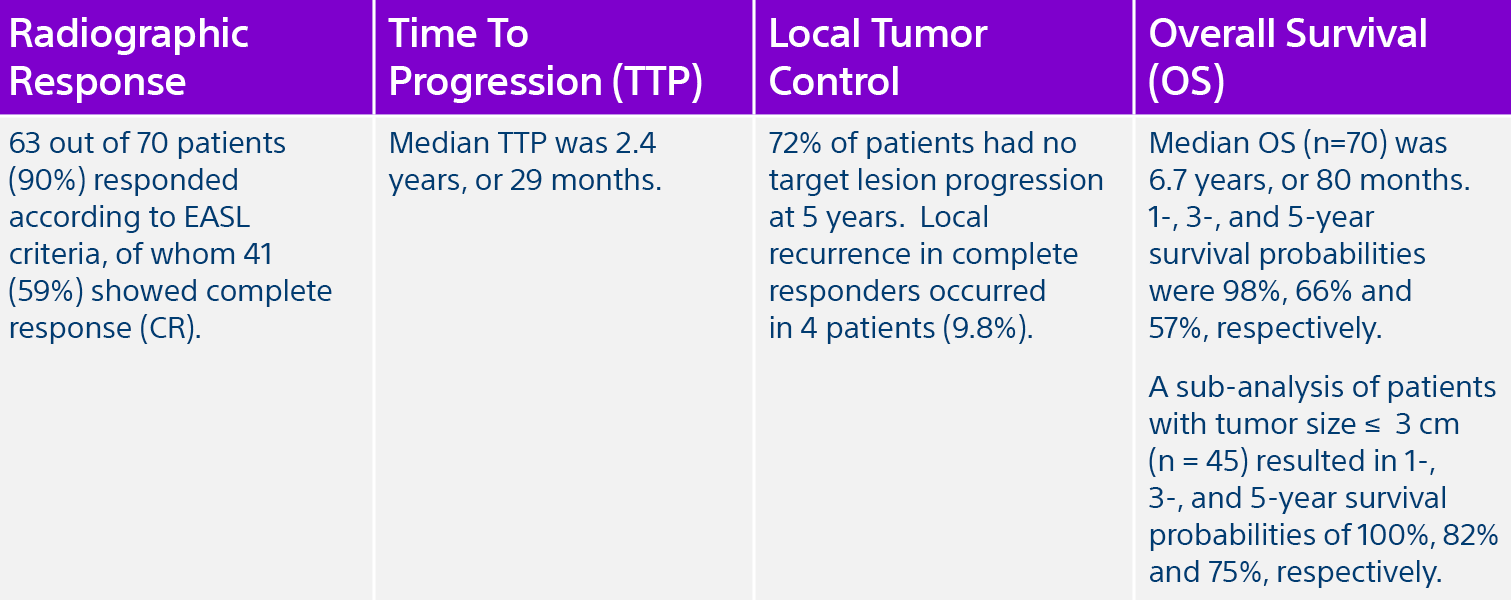
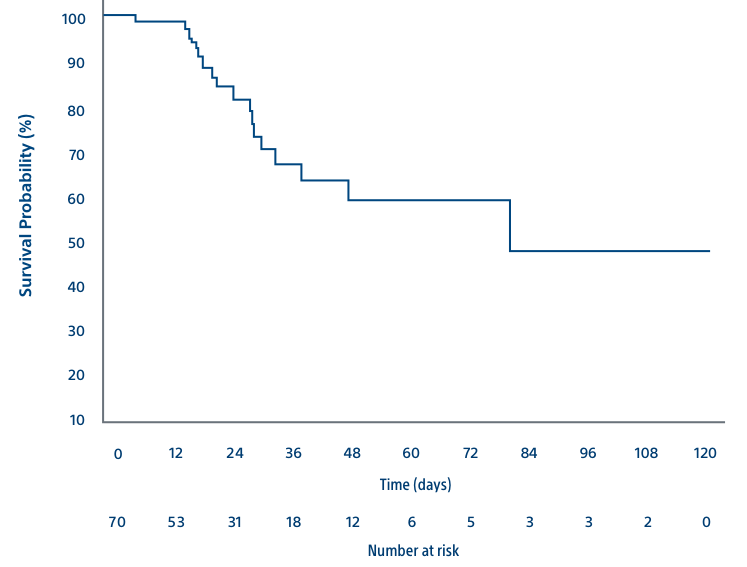
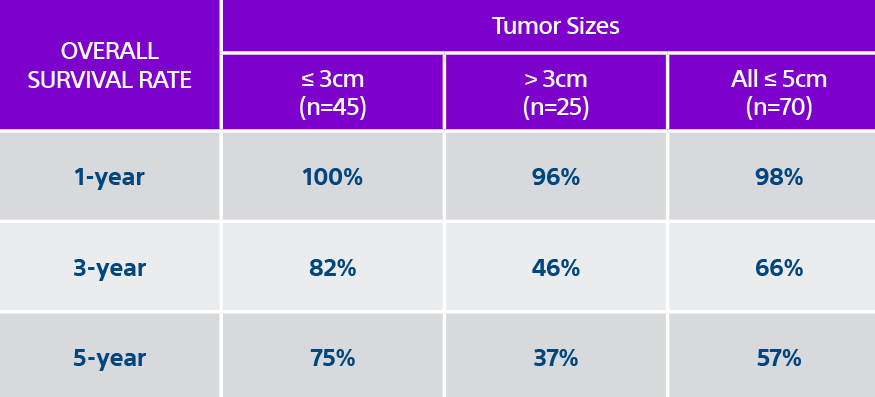
*RF ablation shows similar reported survival outcomes to resection and transplantation for HCC ≤ to 3 cm
BCLC = Barcelona Clinic Liver Cancer; HCC= hepatocellular carcinoma; RF= radiofrequency; EASL= European Association for the Study of the Liver
1. Bruix J, Reig M, Sherman M. Evidence-based diagnosis, staging, and treatment of patients with hepatocellular carcinoma. Gastroenterology 2016;150(4):835–853
2. Riaz A, Gates VL, Atassi B et al. Radiation segmentectomy: a novel approach to increase safety and efficacy of radioembolization. Int J Radiat Oncol Biol Phys 2011;79(1):163–171
3. Vouche M, Habib A, Ward TJ et al. Unresectable solitary hepatocellular carcinoma not amenable to radiofrequency ablation: multicenter radiology-pathology correlation and survival of radiation segmentectomy. Hepatology 2014;60(1):192–201
4. Vouche M, Lewandowski RJ, Atassi R et al. Radiation lobectomy: time-dependent analysis of future liver remnant volume in unresectable liver cancer as a bridge to resection. J Hepatol 2013;59(5):1029–1036