ClinicalEVIDENCE Newsletter 2023 #4 – September 2023
Welcome to the ClinicalEVIDENCE newsletter, your go to source for the latest clinical data on heart diseases, diagnostics, and monitoring.
Our aim is to provide you with cutting-edge information that will keep you up-to-date on the most recent advancements in the field of heart failure management.
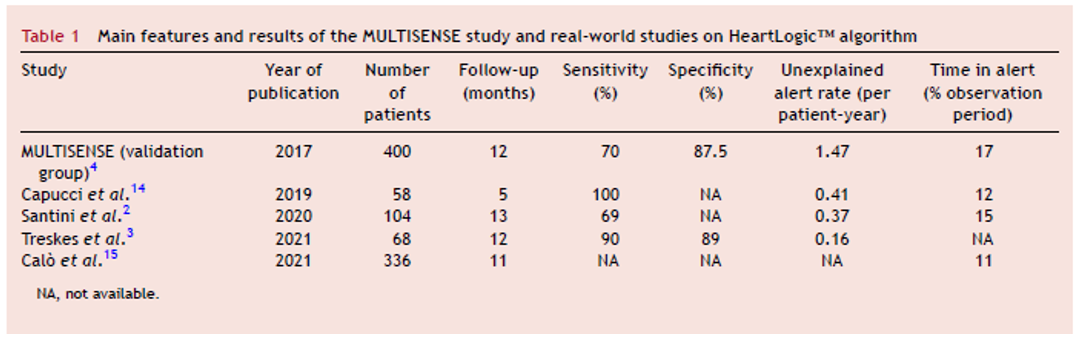
to have the opportunity to share the key messages of the latest HeartLogicᵀᴹ and Remote Monitoring publications.
We will also provide you with the highlights of the abstracts presented at the most important European Congress of Cardiology held in Amsterdam last August.