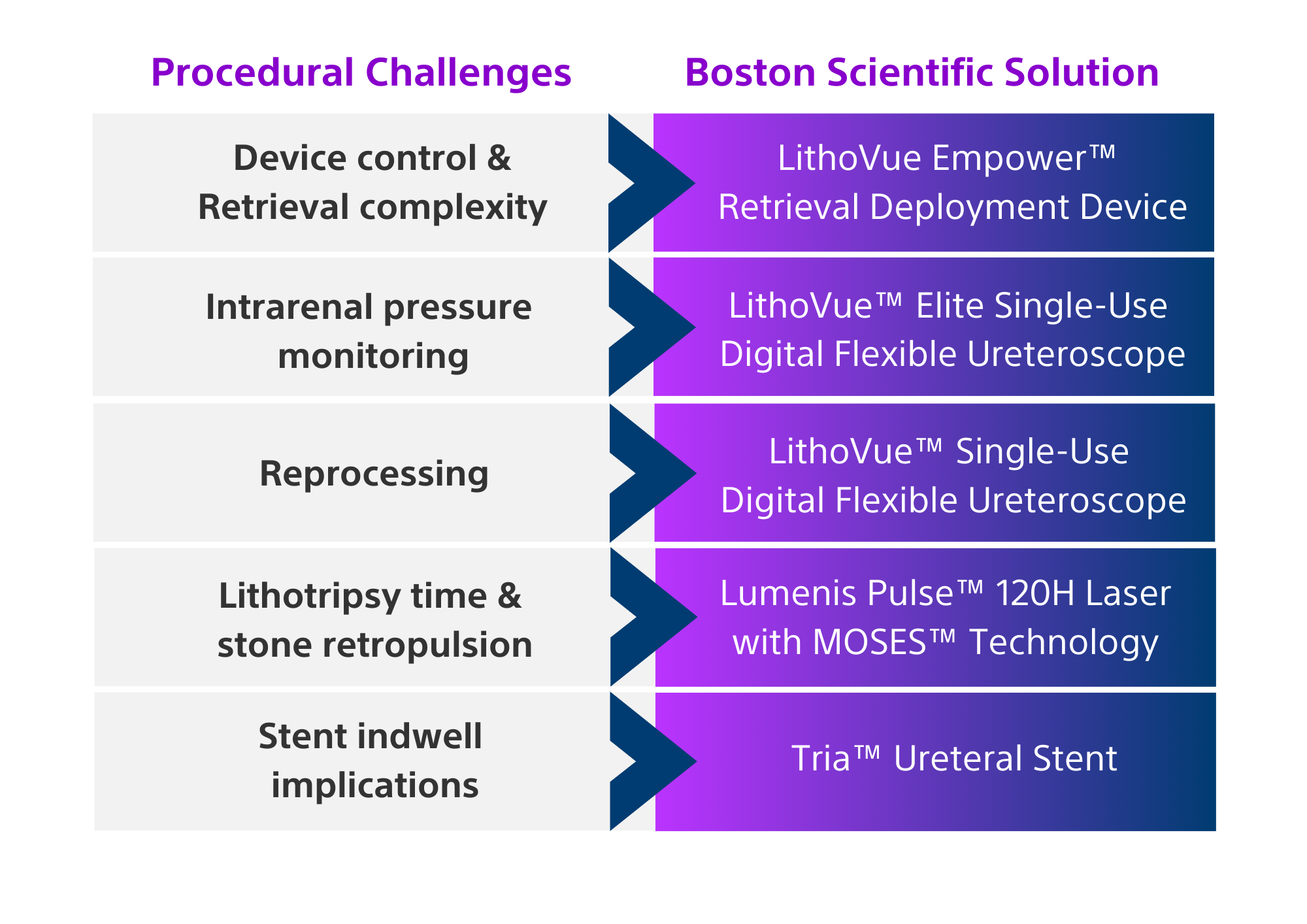
*The MOSES™ Technology is inclusive of both MOSES 1.0 and MOSES 2.0 settings and features.
**Scope 1 emissions are direct emissions from owned or controlled sources.
Scope 2 emissions are indirect emissions from the generation of purchased energy.
Scope 3 emissions are all indirect emissions (not included in scope 2) that occur in the value chain of the reporting company, including both upstream and downstream emissions.
† Bench Test results may not necessarily be indicative of clinical performance. Testing performed on behalf of BSC. Study methodology: Testing was performed by an independent third party using the in-vitro BEST™ method to evaluate salt adhesion of the ureteral stents. A total of 30 samples from each ureteral stent family were tested in both a sterile Artificial Urine Model and a Bacterial Infection Model (n=15 in each model) for 2 weeks. Proteus mirabilis was used as the microbial challenge in the Bacterial Infection Model due to its known urease production and involvement in struvite formation.
‡Bench Test results may not necessarily be indicative of clinical performance. Reduction in stent durometer represents the average percent drop in stent durometer from 25°C to 37°C in air.
Kidney stone pictures are for illustrative purposes only. Source: Getty Images and Adobe Stock.
References
1. Data on file with Boston Scientific.
2. Mager R, et al. Clinical outcomes and costs of reusable and single-use flexible ureterorenoscopes: a prospective cohort study. Urolithiasis. 2018 Nov;46(6):587-593.
3. Joice GA, et al. Ergonomics and procedure time of novel retrieval deployment device for single surgeon ureteroscopy. Abstract presented at EUS Annual Meeting, May 18, 2018, San Francisco, CA
4. Ibrahim A, et al. Double-Blinded Prospective Randomized Clinical Trial Comparing Regular and Moses Modes of Holmium Laser Lithotripsy. J Endourol. 2020 May;34(5):624‐8.
5. Cinman NM, et al. Associated conditions and treatment of the pelvic kidney. In: Smith AD, Badlani GH, Preminger GM, Kavoussi LR eds. Smith’s Textbook of Endourology. Blackwell Publishing;2012;(62):707-715
6. Elhilali MM, et al. Use of the Moses Technology to Improve Holmium Laser Lithotripsy Outcomes: A Preclinical Study. J Endourol. 2017 Jun;31(6):598-604.
7. Mues AC, et al. Evaluation of 24 holmium:YAG laser optical fibers for flexible ureteroscopy. J Urol. 2009 Jul;182(1):348-54.
8. Carey RI et al. Frequency of ureteroscope damage seen at a tertiary care center. J Urol. 2006 Aug;176(2):607-10.
9. Collins JW, et al. Cost analysis of flexible ureterorenoscopy. BJU Int. 2004 May;93(7):1023-6.
10. Chi T et al. Durability of flexible ureteroscopy and predictors of repair: A prospective multi-center study. Poster session presented at The European Association of Urology Annual Congress; 2016 March; Munich, Germany.
11. Carey RI and Carey MS. The Ureteroscope Matters: Matched Pari Analysis Reveals Increased Operative Time and Reoperation Associated with the Use of Refurbished Flexible Ureterosocpes from a Third Party Out-sourced Vendor. Poster session presented at: Southeast Section American Urological Association Annual Meeting; 24 March 2017; Austin, TX.
12. Hubosky et al. Defining the rate of encountering unacceptable reusable flexible ureteroscopes for immediate clinical use: 'Bad out of the Box.' Poster Session presented at The World Congress of Endourology, September 2017; Vancouver, British Columbia, Canada (MP3-10).
13. Matlaga B. Moving from four hands to two during flexible ureteroscopy with stone manipulation. Abstract presented at the World Congress of Endourology, 2018, Paris
14. Cvetic E. Communication in the perioperative setting. AORN J. 2011 Sep;94(3): 261-70.
15. Gillespie, B. M., et al. Interruptions and Miscommunications in surgery: an observational study. 2012 AORN Journal, 95(5), 576-590.
16. Clark, C. M., & Kenski, D. Promoting civility in the OR: an ethical imperative. 2016 AORN Journal, 105(1), 60-66.
17. Agarwal DK, et al. Catheter removal on the same day of holmium laser enucleation of the prostate: Outcomes of a pilot study. Urology. 2020 Dec;146:225‐9.
18. Tracey J, et al. Ureteroscopic High‐Frequency Dusting Utilizing a 120‐W Holmium Laser. J Endourol. 2018 Apr;32(4):290‐
19. Tokas T, et al. Pressure matters: intrarenal pressures during normal and pathological conditions, and impact of increased values to renal physiology. World J Urol. 2019 Jan;37(1):125-31.
20. Sutcliffe KM, et al. Communication failures: an insidious contributor to medical mishaps. Acad Med. 2004;79(2):186-194.
21. Kawahara T, et al. Ureteral Stent Encrustation, Incrustation, and Coloring: Morbidity Related to Indwelling Times J Endourol. 2012 Feb;26(2):178-82.
22. Ofstead C et al. The effectiveness of sterilization for flexible ureteroscopes: A real-world study. Am J Infect Control. 2017 Aug 1;45(8):888-895.
23. Ofstead CL. Endoscope reprocessing methods: a prospective study on the impact of human factors and automation. Gastroenterol Nurs. 2010 Jul-Aug;33(4):304-11.
24. SM Hession. Endoscope Disinfection by Orthophthalaldehyde in a Clinical Setting An Evaluation of Reprocessing Time and Costs Compared With Glutaraldehyde. Gastroenterol Nurs. 2003 May-Jun;26(3):110-4
25. Park HK, et al. The impact of ureteral stent type on patient symptoms as determined by the ureteral stent symptom questionnaire : a prospective, randomized, controlled study. J Endourol. 2015 Mar;29(3):367-71. 4
26. Davis NF, et al. Carbon Footprint in Flexible Ureteroscopy: A Comparative Study on the Environmental Impact of Reusable and Single-Use Ureteroscopes. J Endourol. 2018 Mar;32(3):214-217.
27. Pfiedler Enterprises. The care and handling of rigid and flexible scopes (an online continuing education activity). Aurora, CO, 2013.
28. Rutala WA., WeberDJ., & Healthcare Infection Control Practices Advisory Committee. Guideline for disinfection and sterilization in healthcare facilities. Atlanta, GA: Centers for Disease Control and Prevention, 2008.
29. Clemens JQ, et al. Joint AUA/SUNA white paper on reprocessing of flexible cystoscopes. The Journal of Urology. 184(6):2241-2245, 2014.
30. Smith DR, et al. Glutaraldehyde exposure and its occupational impact in the health care environment. Environmental Health and Preventive Medicine. 11(1):3-10, 2006.
31. Takigawa T, Endo Y. Effects of glutaraldehyde exposure on human health. Journal of Occupational Health. 48(2):75-87, 2006.
32. Rideout K, et al. Considering risks to healthcare workers from glutaraldehyde alternatives in high-level disinfection. Journal of Hospital Infection. 59(1):4-11, 2005.
33. Olympus Medical Systems Corporation. Uretero-reno videoscope Olympus URF Type V. Japan, 2014.
34. PENTAX Medical Company. Pentax ureteroreno fiberscope FUR-9P. Japan, 2011.
35. Richard Wolf Medical Instruments Corporation. Flexible fiber ureterorenoscopes 7325.071/7325.076. United States, 2013.
36. Stryker Corporation. Stryker ideal eyes HD URT-7000S/7000Si flexible video ureteroscope. United States, 2012.