HeartLogic Performance in Clinical Practice
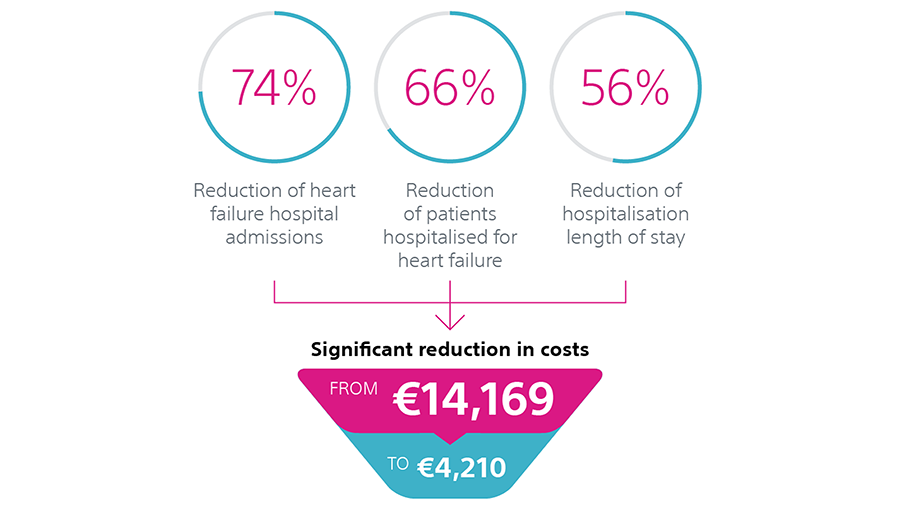
HeartLogic reduces hospitalisations for decompensated heart failure and significantly reduces the costs per patient for the healthcare system, as described in the Heggermont et al publication.1
| MultiSENSE2 (Validation Data Set) |
Capucci et al.3 (ESC HF 2019) |
Santini, Heggermont et al.4 (Clin Card 2020) |
RE-HEART Phase I5 (ESC HF 2020) |
RE-HEART Phase II6 (ESC HF 2020) |
|
|---|---|---|---|---|---|
| PATIENTS | 400 | 58 | 104 | 104 | 215 |
| FOLLOW-UP (MEDIAN) |
12 months | 5 months | 13 months | 8 months | 5 months |
| HF HOSPITALISATION RATE (PER PATIENT-YEAR) |
0.20 | 0.21 | 0.15 | N/A | N/A |
| SENSITIVITY | 70% | 100%* | 69%* | N/A | N/A |
| UNEXPLAINED ALERT RATE (PER PATIENT-YEAR) |
1.47 | 0.41 | 0.37 | 0.25 | 0.13 |
| TIME IN HEARTLOGIC ALERT (%) | 17% | 12% | 15% | N/A | N/A |
Retrospective Analysis: Capucci, et al.
Preliminary experience with the multisensor HeartLogic algorithm for heart failure monitoring: a retrospective case series report
In a real-world scenario, HeartLogic alerts preceded heart failure symptoms by a median of 12 days and HF events by 38 days, which demonstrates the opportunity to identify patients earlier in the time course of HF decompensation.3
Pre-Symptomatic Insights7
| Early Warning Time (Days) |
Maximum HeartLogic Index | |
|---|---|---|
| HF HOSPITALISATIONS | 38 [15-61] | 40 [28-40] |
| HF VISITS | 12 [1-19] | 24 [20-30] |
Sensors with Worsening on the Day of the Alert Threshold Crossing3
| S3 Heart Sounds | S3/S1 Heart Sounds | Night Heart Rate | Thoracic Impedance | Respiration Rate | Rapid Shallow Breathing Index |
|---|---|---|---|---|---|
| 84% | 88% | 60% | 44% | 36% | 36% |
Prospective Analysis: Santini, et al.
Primary Objectives
- Evaluate the clinic workflow of HeartLogic alert management.
- Compare an alert-based, follow-up strategy with scheduled monthly remote transmissions.
- Evaluate the association between HeartLogic alert state and signs and symptoms of worsening heart failure.
Conclusions
- This is the first publication to prospectively evaluate the HeartLogic algorithm in clinical practice utilizing a standardised remote-monitoring protocol.
- This analysis demonstrated HeartLogic alerts to be frequently clinically meaningful and associated with impending HF events.
- The analysis confirmed that the volume of alert-driven, remote follow-ups is low (0.93 per patient-year) when compared with a monthly remote follow-up protocol (10.3 per patient-year) and demonstrates that an alert-based management strategy may be more efficient than a scheduled monthly remote follow-up strategy.
- The probability of detecting common signs and symptoms of HF at regular remote or in-office assessment is extremely low when the patient is out of HeartLogic alert state.
Evaluating the Clinic Workflow of HeartLogic Alert Management
Of the 60 clinically meaningful alerts during the study period, 80% provided new information to clinicians, which highlights HeartLogic’s ability to proactively identify patients at risk.4



“We learned that HeartLogic is very powerful in stratifying patient with a very low risk. When we have a patient in an out-of-alert condition, we can also give the attention to other patients.”
Luca Santini, MD
RE-HEART Registry Phase I
Preliminary Results of the Spanish Multicentric HeartLogic (RE-HEART) Registry: A Blinded Analysis
Phase 1 of the RE-HEART Registry was a retrospective, blinded analysis designed to analyze the association between clinical events and HeartLogic alerts in patients from 12 Spanish centers.
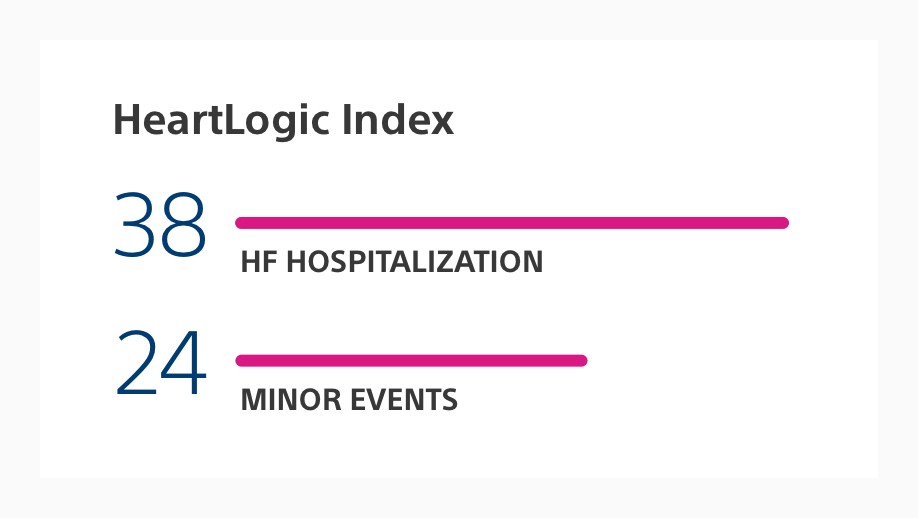
Maximum HeartLogic Alert Index5
The RE-HEART Registry analysis found a longer duration of alert and higher maximum HeartLogic index for patients with heart failure hospitalisations compared to those with minor events.
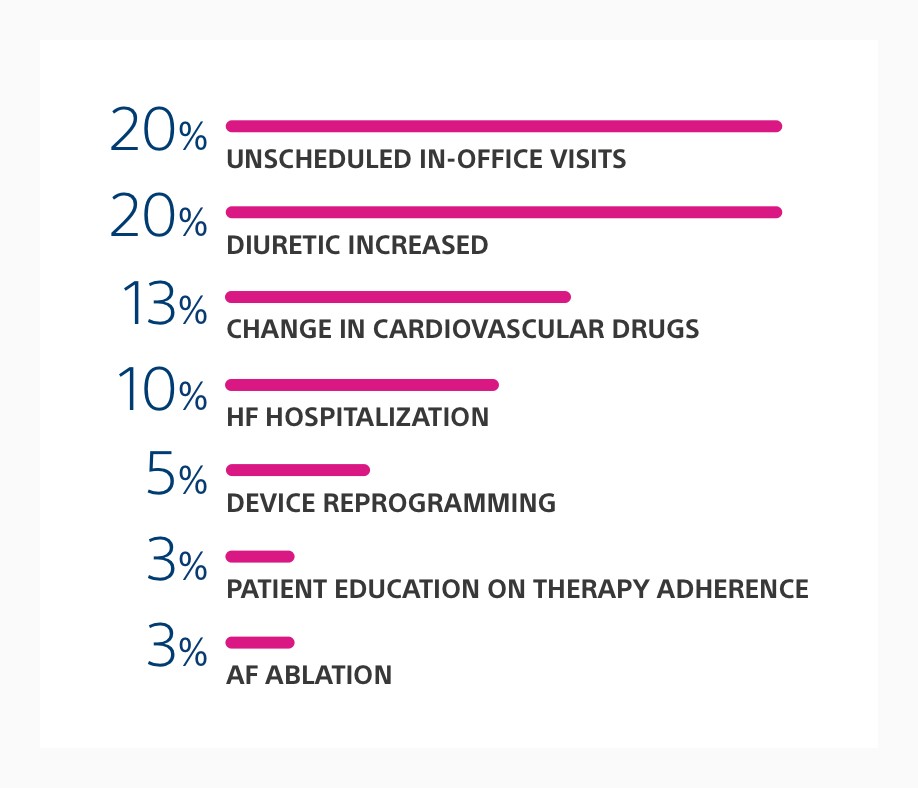
RE-HEART Registry Phase II
Preliminary Results of the Spanish Multicentric HeartLogic (RE-HEART) Registry: Adoption of an Alert-Based Heart Failure Management Approach
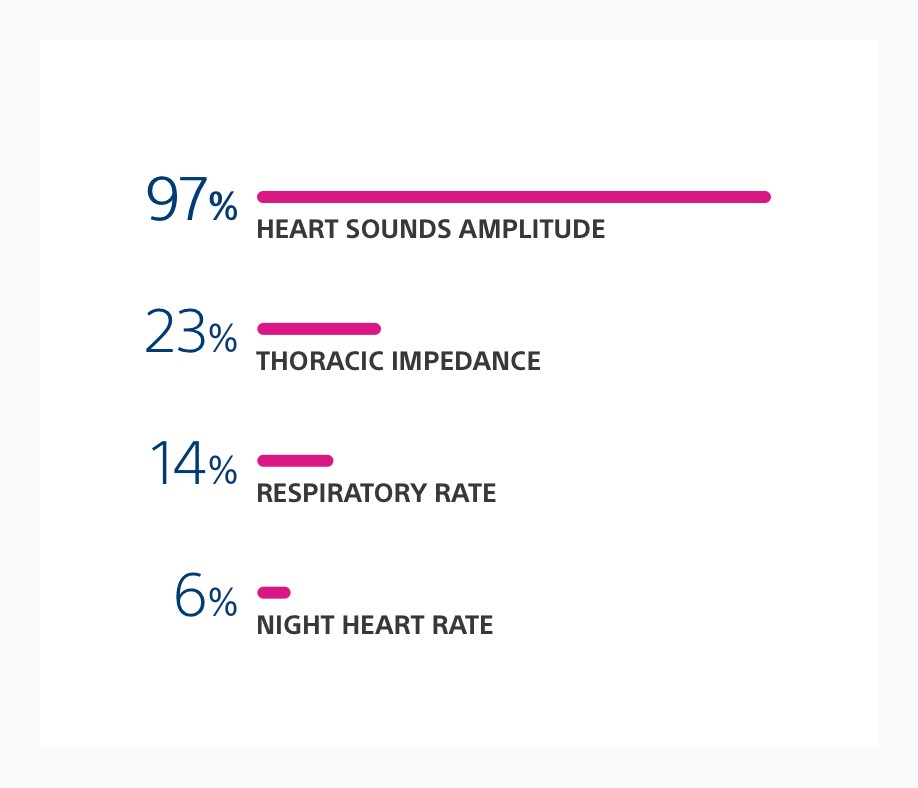
Phase II of the RE-HEART Registry showed a diverse array of interventions were taken for a diverse patient population. HeartLogic contributing sensors at time of alert were primarily driven by heart sounds.
Sign up for periodic emails and receive a HeartLogic fact sheet to share with your patients’ care teams.
Get Phase I results from this global trial evaluating the integration of HeartLogic into clinical practice.
Find out how HeartLogic helps you see patients’ physiologic responses to arrhythmic and pacing changes.