Rotablator™ Case Study: Calcified Plaque
Rotational Atherectomy System
Diagnosis
- EKG demonstrated sinus bradycardia with an old inferior infarct.
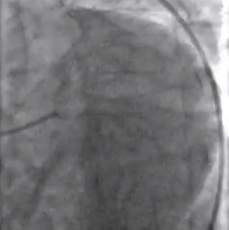
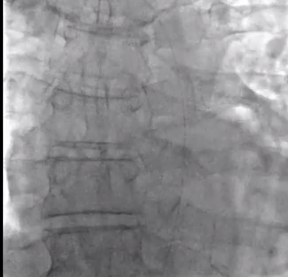
- Left coronary angiogram demonstrated separate ostia of LAD and left circumflex arteries.
- The left circumflex artery had TIMI-2 flow. There was a high grade, sub-total stenosis in its proximal portion.
- With some difficulty, a 6 F extra back-up guide catheter was used to cannulate the left circumflex.
Procedure
- A workhorse coronary wire was successfully advanced across the lesion.
- Predilatation with a 2.0 x 12 mm RX semi-compliant balloon was attempted, but was unsuccessful because it could not cross the lesion.
- Predilatation was successful with a 1.5 x 12 mm Apex® Push balloon; subsequent angiogram demonstrated restoration of TIMI-3 flow.
- Further predilatation was then performed with a 2.5 x 12 mm NC Quantum Apex™ MR balloon at high pressure. There was clear under expansion of the balloon by fluoroscopy.
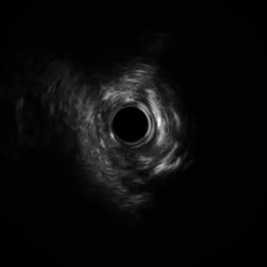
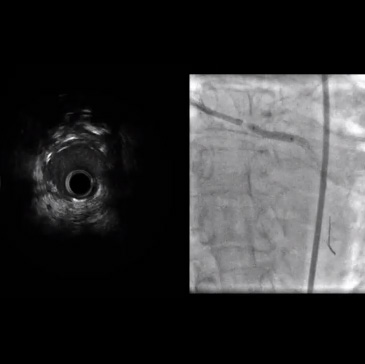
- Intravascular ultrasound showed a highly narrowed vessel with substantial fibro-calcific plaque. Given these findings, the decision was made to proceed with Rotablator.
- The original wire was exchanged over an OTW balloon for a RotaWire™ Floppy Guide Wire.
- A 1.5 mm burr was advanced and rotational atherectomy was performed. This was followed by further high pressure dilatation with an NC Quantum Apex balloon with poor expansion.
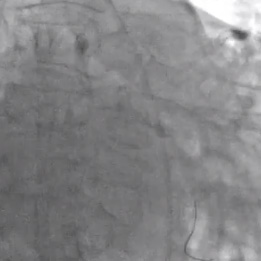
- Subsequent angiography showed TIMI-3 flow with no dissections, but still a residual significant stenosis.
- Given the need for further rotational atherectomy with a larger burr, the decision was made to perform a guide exchange for an 8 F guide catheter.
- The RotaWire Floppy Guide Wire was exchanged for a 300 cm extra support wire using an OTW system.
- The 6 F guide and sheath were then walked out over the extra support wire.
- An 8 F sheath and guide were re-advanced over the extra support wire.
- The extra support wire was then exchanged for the RotaWire Extra Support wire to bias atherectomy within the plaque.
- Rotablator was then performed with a 2.0 mm Rotablator burr.
- The lesion was assessed and pre-dilated at high pressure with a 3.25 x 15 mm NC Quantum Apex balloon.
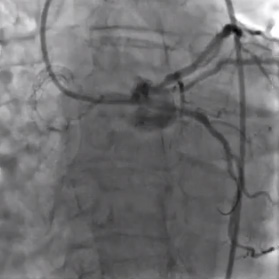
- A 3.5 x 16 mm PROMUS Element™ stent was deployed with excellent expansion by fluoroscopy.
- Post stent intravascular ultrasound showed focal under expansion in the proximal portion of the stent.
- Post-dilatation was then performed at high pressure with a 3.75 x 12 mm NC Quantum Apex balloon.
- Final angiography demonstrated TIMI-3 flow, no dissections, and no residual stenosis in the left circumflex system.
Result*
- Rotational atherectomy allowed for substantial plaque modification that enabled successful balloon predilatation and stent deployment.
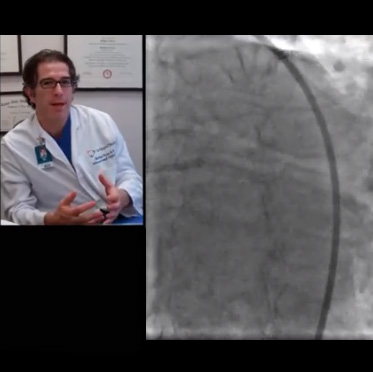
Physician Commentary
"I think this case demonstrates that it is important to have rotational atherectomy in your tool kit for cases where you do not get adequate predilatation or stent deployment. In this particular case, there was a very aggressive fibro-calcific plaque that was really resistant to even high pressure dilatation with a non-compliant balloon. We were able to do rotational atherectomy, which is a life-saver when you get in this kind of situation."